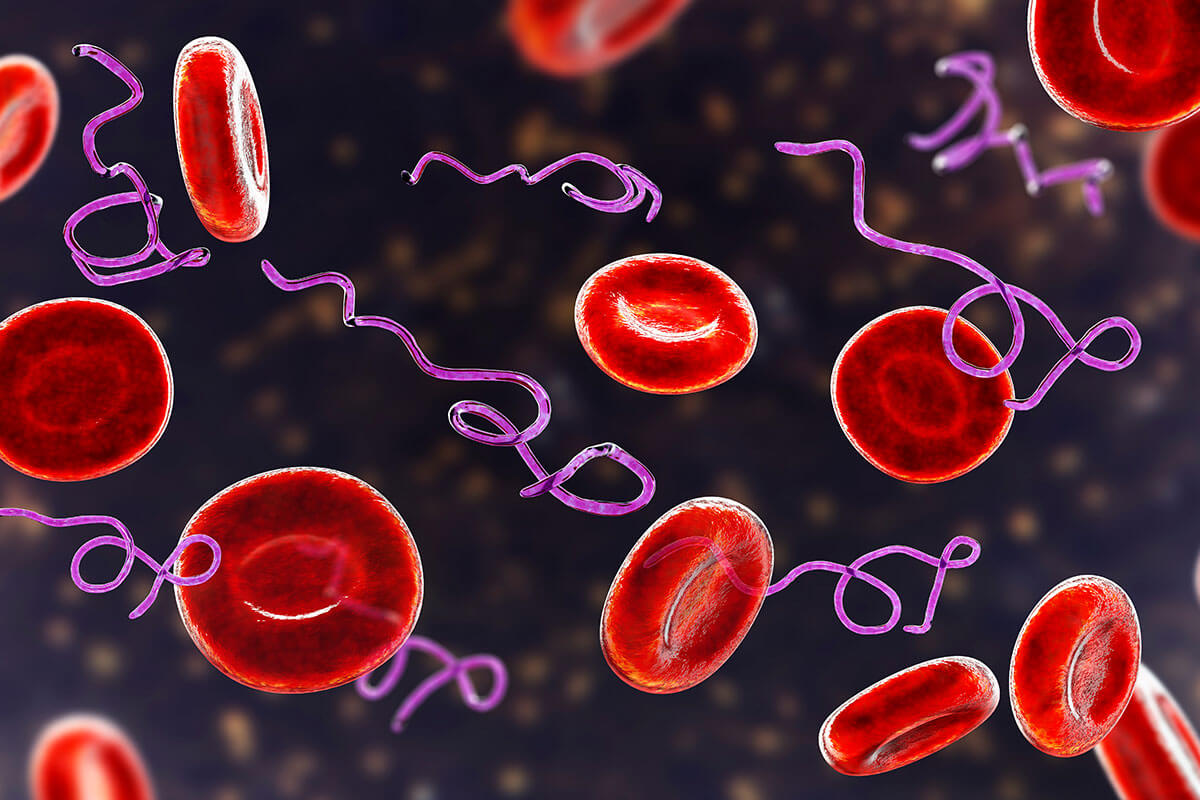
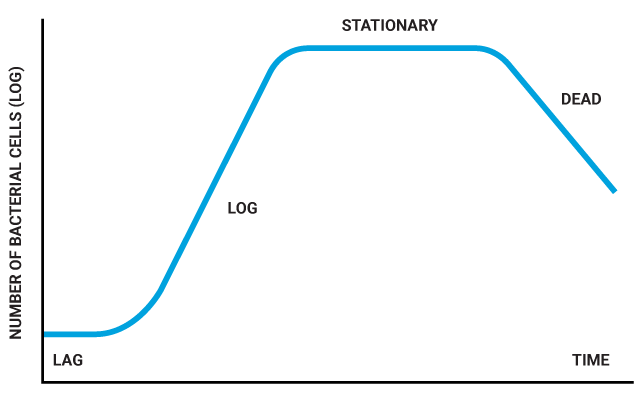
Early in an infection, bacteria are in a growth phase where they divide rapidly to increase the number of bacteria to establish an infection. Bacteria then enter a stationary phase where bacterial growth slows down. The current antibiotic treatments for acute and chronic Lyme Disease and Bartonella primarily work in the bacterial growth phase. Still, these antibiotics are ineffective once the bacteria enter into the stationary phase. In recent years, researchers have conducted screening studies of drugs and natural compounds to identify effective treatments for Lyme Disease and Bartonella in a stationary phase. Surprisingly, a medication called methylene blue proved to be an effective treatment for stationary phase Lyme Disease and Bartonella.

What is Stationary Phase Lyme Disease and Bartonella
There are four phases of bacterial growth – lag, log (growth), stationary, and death. The lag phase is when the bacteria are preparing resources to grow. The log or exponential growth phase is when bacteria are rapidly dividing – one becomes two, two becomes four, four becomes eight, etc.). In the stationary phase, the rate of bacterial growth equals bacterial death, so there is no net change in the number of bacteria. The death phase is when the bacteria die off at a rate that exceeds bacterial growth.
“The conditions that sustain constant bacterial growth are seldom found in nature… The influence of harsh environmental factors, accumulation of toxic metabolic waste products during starvation, and antibiotics – all this threatens the survival of E. coli and other bacteria. For protection against harsh environmental influences, bacterial culture can enter a stationary phase where its internal systems of protection against stress become activated.” Survival guide: Escherichia coli in the stationary phase
Is it Post Treatment Lyme Disease Syndrome (PTLDS) or Chronic Lyme Disease (CLD)?
Lyme disease’s most controversial debate is whether or not the bacteria that causes Lyme disease (Borrelia burgdorferi) survives the commonly prescribed antibiotic regimens and continues to cause symptoms. The Infectious Disease Society of America (IDSA) refers to this phenomenon as Post Treatment Lyme Disease Syndrome (PTLDS). It suggests the infection with Lyme Disease has been adequately treated, and the symptoms remain due to another cause, such as an autoimmune response.
Several research studies have demonstrated the Lyme spirochete persists in humans following antibiotic therapy. The International Lyme and Associated Disease Society (ILADS) characterizes the persistence as Chronic Lyme Disease (CLD). Lyme Disease may persist and become chronic because the commonly used treatments are not effective at treating the stationary phase of the Lyme bacteria.
Stationary Phase of the Lyme Spirochete Causes More Severe Symptoms
In 2018 researchers from John Hopkins University published a study that looked at the severity of arthritis when the bacteria that causes Lyme Disease was in the growth phase, the stationary phase, and biofilm colonies. The research discovered the arthritis was more severe earlier in an infection in the stationary phase and biofilm groups than in the growth phase group. The researchers also concluded that currently used antibiotic regimens are less effective against the stationary and biofilm bacteria.
The currently used antibiotic regimens to treat Lyme Disease kill bacteria in the growth phase, but the bacteria that cause more severe symptoms are not affected.
Methylene Blue for Lyme Disease
In 2014, researchers from Johns Hopkins University screened an FDA drug library for activity against Borrelia burgdorferi (the bacteria that causes Lyme disease). They identified 165 hits (drugs) with higher activity against Lyme disease than doxycycline and amoxicillin. The following year the same researchers narrowed the results down to the top 52 drugs that can be used in humans and effectively killed at last 65% of stationary phase bacteria.
The researchers discovered that various drugs used to treat other infections – including antibiotics, antivirals, antifungals, and antiparasitics – were effective at killing stationary phase Borrelia. One of the top hits was a medication called methylene blue. Methylene blue was originally an antimalarial medication currently used to treat a condition called methemoglobinemia and urinary tract infections. Methylene blue was almost as effective as daptomycin – a drug that has received attention for its ability to treat persistent Lyme disease.
Methylene Blue for Bartonella
An infection with the bacteria Bartonella may be more problematic than Lyme disease. Multiple vectors transmit Bartonella, diagnostic testing historically has not been accurate, and most physicians are not familiar with this infection, so rarely consider it as a diagnosis. If a Bartonella diagnosis is confirmed, a critical challenge is finding effective treatments. The commonly used antibiotics to treat Bartonella – rifampin, azithromycin, clarithromycin, ciprofloxacin, and doxycycline – work early in infection during the bacterial growth phase but are not effective during the stationary phase leading to poor treatment response. It is common for someone to feel better on these medications then have symptoms return as soon as the medications are discontinued due to bacterial resistance.
In 2019, some of the same researchers from Johns Hopkins University who performed the above Lyme disease study completed a drug screen to identify effective medications against the stationary phase Bartonella. Their research discovered 110 drug candidates from an FDA approved drug library that had better activity against Bartonella’s stationary phase than ciprofloxacin. The top 52 drug candidates from the primary screen were evaluated for their effectiveness by the number of bacteria remaining under microscopy. Similar to the previous drug screen findings for stationary phase Lyme disease, only 25% of stationary phase Bartonella bacteria remained following exposure to methylene blue.
The researchers confirmed their findings by performing minimal inhibitory concentrations (MIC) study – the minimum amount of medication need to kill growing bacteria. Again, methylene blue performed very well. Interestingly, the drug daptomycin performed well against stationary phase Bartonella but was not effective against growing Bartonella. Rifampin – a commonly used antibiotic for Bartonella – worked well against growing Bartonella but was not effective at killing Bartonella’s stationary phase.
Another challenge the researchers conducted was to test the effectiveness of the top 7 drugs from a stationary phase culture against Bartonella at various stages of growth to mimic the course of a natural infection. Here, the drugs were evaluated for their effectiveness against 1-day old growth phase 5-day old stationary phase. Again, methylene blue was a top performer proving its effectiveness against Bartonella in the infection’s growth and persistent stages.
Drug Combinations for Treating Bartonella
Researchers published the first study to evaluate drug combinations against Bartonella in the stationary phase and biofilms in 2020. Again, a team of researchers led by Ying Zhang, MD from Johns Hopkins University, expanded upon the single drug screen study from 2019. This research study evaluated the top-performing drugs from the 2019 trial and created 25 two-antibiotic combinations to test their efficacy against Bartonella in the stationary phase and biofilms.
Of the 25 combinations of antibiotics, four were able to completely eradicate stationary phase Bartonella in 24 hours – azithromycin/ciprofloxacin, azithromycin/methylene blue, rifampin/ciprofloxacin, and rifampin/methylene blue.
The next test was to determine how long it took for single and combination antibiotics to kill stationary phase Bartonella. Of the single and combination antibiotics, the methylene blue combinations with azithromycin and rifampin killed Bartonella’s stationary phase in the shortest time.
Biofilms are colonies of bacteria in a structure that improve the survival of the bacteria. In this same study, the researchers experimented to see how much bacteria in biofilms remained after exposure to single and combination antibiotics at two days, four days, and six days. None of the single or combination antibiotics were able to kill Bartonella after 2 and 4 days. However, the azithromycin/ciprofloxacin, azithromycin/methylene blue, rifampin/ciprofloxacin, and rifampin/methylene blue combinations eradicated Bartonella in biofilms after six days.
Given the toxicity of ciprofloxacin, the combinations with methylene blue are a better option for treating Bartonella in the stationary phase and in biofilms.
New Research, New Effective Treatment Options
Treatment options for chronic infections with Lyme disease and Bartonella have historically been inadequate. Recent research using drug screens to identify effective treatments for the stationary phase of infection has produced some promising options. The research has also confirmed the currently used antibiotics primarily work in the initial growth phase of an infection but not the stages that develop in chronic infection. Methylene blue is a promising treatment option for tens of thousands of people suffering from chronic Lyme disease and Bartonella.